1Department of Gastroenterology, Ersta Hospital, Stockholm, Sweden.
2Department of Endoscopy, The Jikei University School of Medicine, Tokyo, Japan.
Corresponding author: [email protected]
During colonoscopy, when confronted with a finding in the colon or rectum the endoscopist must rapidly make a presumptive diagnose in order to provide the best treatment to the patient. This requires a good knowledge of the colorectal pathology to accurately interpret the different types of lesions that may me encountered. High-resolution endoscopy aided by NBI and chromoscopy gives us a clear image making this interpretation easier. The final decision may be to give immediate endoscopic treatment or to refer the patient for advanced endoscopic therapy or surgery.
Here we are presenting some few cases, commonly observed during colonoscopy.
Case 1
a. A small hyperplastic polyp of the rectum with a typical dome-shaped and pale appearance.
b. No clear visible vessels are seen under NBI. No endoscopic treatment is required.
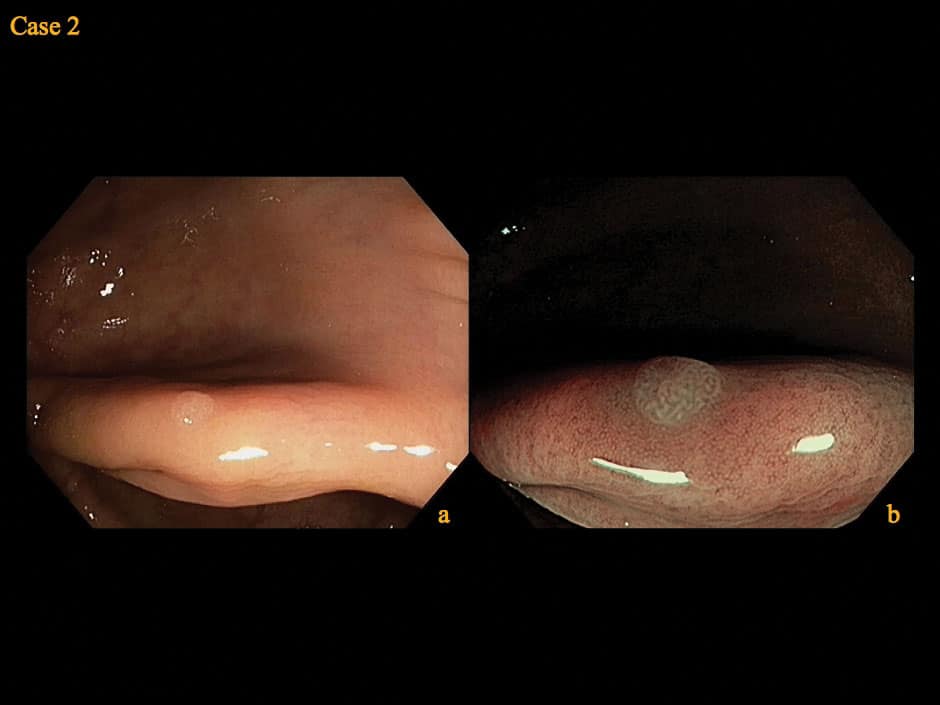
Case 2
a. In the descending colon a small polyp with a pale appearance is observed under white light.
b. NBI demonstrates an adenomatous pattern with linear-shaped openings of the crypts (IIIL pit pattern) as frequently seen in small adenomas. This lesion can easily be treated with a biopsy forceps.
Case 3
a. A small reddish area (arrow) is seen in the transverse colon.
b. Under NBI a well-delimited dark brown spot (suggesting increased angiogenesis) is observed.
c. Chromoscopy reveals a depressed type (IIc) neoplastic lesion with scalloped and well demarcated borders.
d. An opened forceps is used to make obvious the small size of the lesion. This IIc lesion has a high risk of becoming invasive, but due to its small size it can easily be treated by several endoscopic methods including biopsy forceps, hot biopsy but preferably mucosectomy.
Case 4
a. A small elevated lesion is observed in the sigmoid colon near a diverticulum.
b-c. Close-up view under white light and NBI reveal concentric folds surrounding the lesion. No clear vascular pattern is seen under NBI. d. Chromoscopy displays a lesion with the same appearance as the surrounding normal mucosa depicting a normal aerae colonicae. An everted diverticulum is diagnosed.
Case 5
This patient was referred to our unit at Ersta for further endoscopic treatment. At previous endoscopy a reddish area was observed in the transverse colon and multiple biopsies were taken revealing a tubular adenoma with low grade dysplasia.
a. Under white light a flat lesion (IIa) with scarring was detected.
b. NBI shows a regular vascular network with mild dilatation of capillaries indicating a non-invasive neoplastic pattern.
c-d. Under chromoscopy several scars within and outside the lesion are evident and a type IIIL pit pattern compatible with adenoma is observed.
e-f. Mucosectomy was attemped by injecting hypertonic saline in to the submucosal space but due to the scarring a proper lift was not achieved. Endoscopic treatment had to be postponed and the patient rescheduled. The lesion was finally resected by endoscopic submucosal dissection.
Case 6
a. A thickened fold is observed in the ascending colon.
b. NBI shows multiple dilated but regularly distributed crypt openings at the upper left and a darkened area with increased vascularity at the lower right (arrow).
c. Close-up view of the darkened area under NBI demonstrates an adenomatous pattern. A scar after previous biopsy is obvious. Dilated glands are seen below the scar (arrow). A sessile serrated polyp with adenomatous changes was diagnosed. Sessile serrated polyps with adenomatous changes can rapidly undergo malignant transformation and endoscopic treatment is therefore mandatory.